Physician Contract Review: Essential Steps Before Signing

Most physicians now practice as employees, not independent owners. The AMA estimates that around 90% of new physicians sign employment contracts rather than start their own practices, which means your agreement is one of the biggest financial and career decisions you’ll make.
A careful physician contract review helps you understand what you’re really agreeing to: your pay, call schedule, non-compete limits, malpractice coverage, and your exit options if things change. Done well, it protects not just your income, but also your license, reputation, and flexibility to change jobs later.
This guide walks through a clear, step-by-step physician contract review checklist so you know what to look for, what’s negotiable, and when to bring in a healthcare attorney to back you up.
Table of Contents
- Table Of Contents
- Quick Summary
- What Is A Physician Contract Review?
- Why Careful Contract Review Matters For Physicians
- Step-By-Step Physician Contract Review Checklist
- Step 1: Clarify Your Role, Duties, And Schedule
- Step 2: Break Down Compensation And Bonuses
- Step 3: Analyze Restrictive Covenants Non-Compete Non-Solicit Confidentiality
- Step 4: Confirm Malpractice Coverage And Tail Obligations
- Step 5: Check Term Termination And Renewal Clauses
- Step 6: Review Compliance, Stark Law, And Anti-Kickback Risks
- Step 7: Evaluate Benefits, Support, And Career Development
- Step 8: Decide What To Negotiate And When To Call An Attorney
- Common Mistakes Physicians Make With Contracts
- Costs, Timelines, And How Professional Review Works
- Protect Your Career With Confident Contract Review
- Frequently Asked Questions
- Recommended
Quick Summary
| Takeaway | Explanation |
|---|---|
| Your contract is a long-term career decision | It controls your pay, hours, call, location, and exit options for years; a sloppy review can cost six figures over time. |
| Duties and compensation must be crystal clear | Make sure the agreement spells out sites, hours, RVU or productivity formulas, bonuses, and when/why pay can change. |
| Non-competes and tail coverage are often the most expensive surprises | Broad non-competes and unfunded tail insurance can restrict your future or cost tens of thousands when you leave. |
| Compliance language can affect your license | Terms tied to referrals, Stark, or Anti-Kickback rules must be structured carefully to avoid regulatory risk. |
| Many terms are negotiable | Call schedule, signing bonuses, repayment clauses, and restrictive covenants are frequently adjusted when physicians push back. |
| Expert legal review is fast and affordable | Flat-fee services like AirCounsel’s physician contract review give you a line-by-line analysis, usually within 2 business days. |
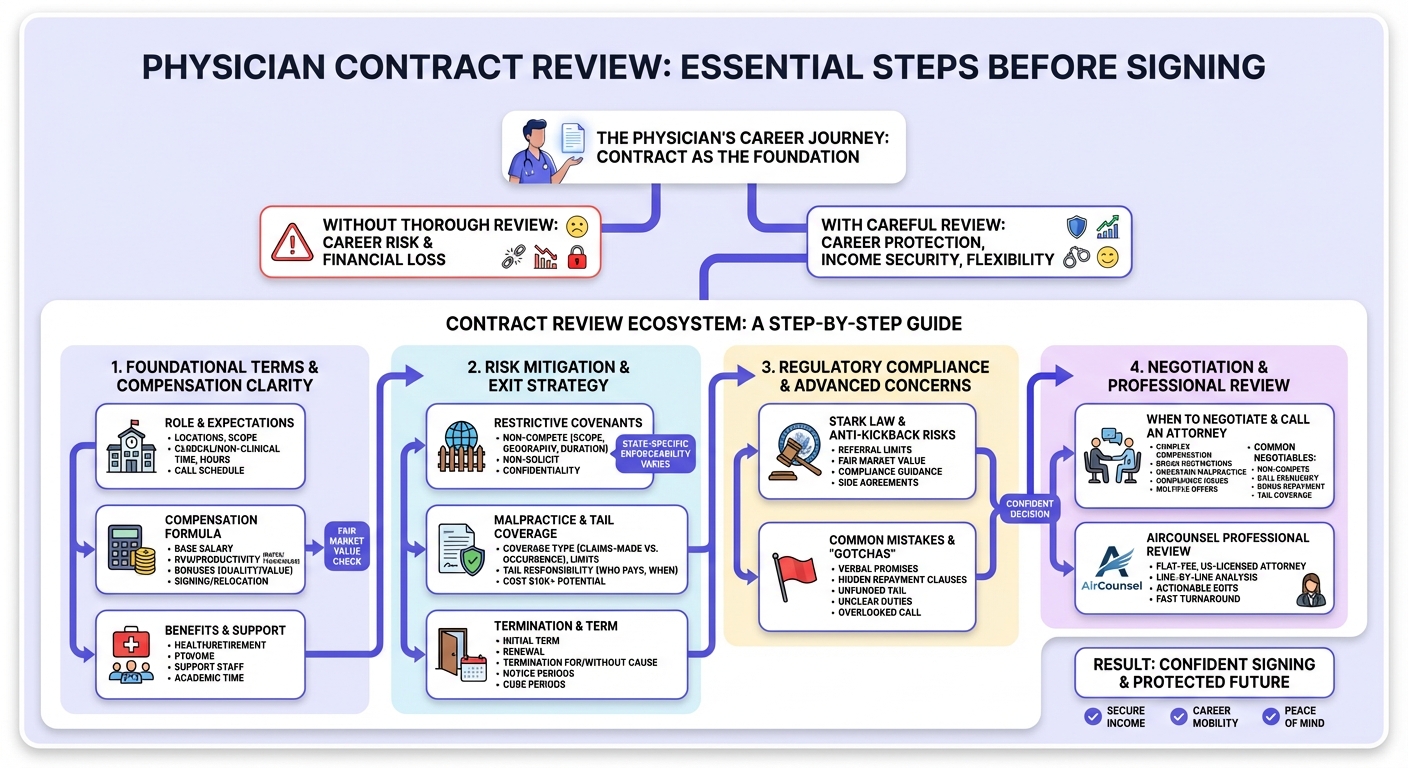
What Is A Physician Contract Review?
A physician contract review is a detailed legal and business analysis of your employment (or independent contractor) agreement before you sign it.
It typically covers:
- Your role: duties, locations, call, and performance expectations
- Compensation: salary, productivity bonuses, and how they’re calculated
- Risk: malpractice coverage, tail, indemnity, and termination rights
- Restrictions: non-compete, non-solicit, and confidentiality clauses
- Compliance: how the agreement fits with federal and state healthcare laws
The goal is not just to understand the words on the page, but to translate them into real-world consequences for your income, work-life balance, mobility, and license.
Why Careful Contract Review Matters For Physicians
Physician agreements are different from standard employment contracts. They intersect with:
- Complex compensation formulas (RVUs, collections, quality metrics)
- Hospital bylaws, medical staff rules, and call coverage obligations
- Federal laws like Stark (physician self-referral) and the Anti-Kickback Statute
- State-specific rules on non-compete clauses, licensure, and scope of practice
Professional bodies like the AMA highlight how contract terms on duties, compensation, and restrictive covenants can significantly shape your practice trajectory and satisfaction.
Done well, your physician contract review should:
- Confirm that the offer matches what was promised verbally
- Reveal red flags and “gotchas” that could trap you later
- Show you what’s realistically negotiable in your specialty/market
- Give you a strategy and language for negotiating better terms
Step-By-Step Physician Contract Review Checklist
Step 1: Clarify Your Role, Duties, And Schedule
Start with how you will actually spend your days.
Look for:
- Practice locations: Every facility, clinic, or satellite site where you may work
- Specialty/scope: Are you limited to certain procedures, age groups, or service lines?
- Clinical vs. non-clinical time: Admin, teaching, research, leadership roles
- Hours and shifts: Clinic hours, expected patient volume, hospital coverage
- Call schedule: Frequency, in-house vs. home call, post-call days, backup expectations
Ask yourself:
- Is the role described the same as what you discussed in interviews?
- Could you be reassigned to undesirable locations or schedules without your consent?
- Is there any protection against unreasonable increases in duties or call?
If any of this is vague (“as assigned by Employer”), that’s a sign to tighten language or negotiate clearer boundaries.
Step 2: Break Down Compensation And Bonuses
Compensation is often complex in physician contracts. Carefully review:
- Base salary: Amount, duration (e.g., guaranteed for 1–2 years), and when it resets
- Productivity pay: RVU conversion rates, collection thresholds, and formulas
- Quality or value-based bonuses: Metrics used, who sets them, how often they’re revised
- Signing bonus and relocation: Payout schedule and any repayment obligations
- Incentive changes: Employer’s ability to unilaterally change compensation models
A simple way to organize your review:
| Compensation Element | What To Confirm | Common Pitfall |
|---|---|---|
| Base Salary | Amount, guarantee length, review dates | Salary dropping sharply after year 1 without clear criteria |
| RVU / Productivity | RVU rate, how RVUs are counted, caps | Changing RVU targets mid-year; unclear “wrvu” definitions |
| Bonuses | Metrics, timing, clawback terms | Bonus tied to metrics fully controlled by employer |
| Signing / Relocation | Vesting period, repayment triggers | Repayment of full bonus even after partial service |
| Other Income | Medical directorship, call stipends | Extra duties added later with no extra pay |
Check whether total compensation is consistent with fair market value in your specialty and region. If pay seems unusually high or low, it may raise compliance questions or indicate future pay cuts.
Step 3: Analyze Restrictive Covenants Non-Compete Non-Solicit Confidentiality
Restrictive covenants can affect your options long after you leave.
Review:
- Non-compete:
- Geographic radius (e.g., 10–25 miles)
- Duration (e.g., 1–2 years)
- Scope (inpatient, outpatient, telehealth, subspecialty)
- Non-solicitation: Limits on contacting patients, staff, or referral sources after you leave
- Confidentiality: How broadly “confidential information” is defined and for how long
Key points:
- Enforceability of physician non-competes varies by state; some are strongly limited, others routinely enforced.
- Even where enforceable, these clauses can often be narrowed through negotiation (less distance, shorter term, limited to specific sites or departments).
- Very broad non-solicits can block you from hiring even non-clinical staff or working with referring providers.
If you plan to stay in the same city long term, this section is critical.
Step 4: Confirm Malpractice Coverage And Tail Obligations
Malpractice coverage details are often buried but can be very expensive if misunderstood.
Check:
- Type of coverage: Claims-made vs. occurrence
- Who pays premiums: Employer, you, or shared
- Tail coverage (for claims-made policies):
- Who is responsible for purchasing tail if you leave
- What happens if you are terminated “for cause” vs. “without cause”
- Coverage limits: Per-claim and aggregate limits; whether they meet local norms
Tail coverage can cost 1–2 times your annual premium, sometimes tens of thousands of dollars. Make sure you know:
- Whether the employer will pay for tail if they terminate you without cause
- Whether you forfeit tail coverage if you leave early or join a competitor
- If there’s any repayment obligation if you depart within a set period
Step 5: Check Term Termination And Renewal Clauses
Next, look at how easily each side can end the relationship.
Focus on:
- Initial term: Commonly 1–3 years
- Automatic renewal: Does the contract roll over unless you give notice?
- Termination without cause:
- Is it allowed by either party?
- Notice period (e.g., 60–180 days)
- Termination for cause:
- Grounds (loss of license, DEA, hospital privileges, etc.)
- Whether you get a chance to cure certain issues
These clauses drive:
- How trapped you are if the fit is wrong
- How long you must stay after giving notice
- Whether you risk sudden loss of income or malpractice coverage
Look for mismatches, such as the employer having broad “without cause” termination rights while your ability to leave freely is heavily restricted.
Step 6: Review Compliance, Stark Law, And Anti-Kickback Risks
Healthcare employment agreements must also be structured to comply with federal and state regulations.
Two major federal rules to be aware of:
- Stark Law (physician self-referral): Limits physician referrals of Medicare/Medicaid patients to entities where they (or their immediate family) have a financial relationship, unless an exception applies. The Centers for Medicare & Medicaid Services (CMS) provide detailed guidance on physician self-referral under Stark Law.
- Anti-Kickback Statute: Prohibits offering, paying, soliciting, or receiving anything of value to induce referrals for services reimbursable by federal healthcare programs. CMS’s Roadmap for New Physicians on fraud and abuse explains key concepts and risk areas.
While your contract may not cite these laws by name, watch for:
- Incentive structures tied directly to the volume or value of referrals
- Unusually high compensation that seems out of line with fair market value
- Side agreements (e.g., medical directorships) that lack clear duties or time requirements
A healthcare attorney can flag provisions that may create compliance exposure for you or your employer.
Step 7: Evaluate Benefits, Support, And Career Development
Beyond salary, benefits and support can make or break a job.
Review:
- Benefits: Health, dental, vision, disability, life insurance, retirement match
- Paid time off: Vacation, sick days, CME time, parental leave, holidays
- CME and licensure: CME allowance, reimbursement for licenses, DEA, board fees
- Support staff: Access to MAs, scribes, NPs/PAs, call coverage support
- Practice infrastructure: EHR, scheduling, triage, marketing, and referral pipelines
- Academic/research time (if applicable): Protected time and expectations for publications or teaching
A slightly lower salary may be worth it if the practice offers strong staffing, manageable patient volumes, and robust benefits.
Step 8: Decide What To Negotiate And When To Call An Attorney
Not everything in a physician contract is negotiable—but more is negotiable than many residents and attendings realize.
Commonly negotiable areas:
- Non-compete radius and duration
- Call frequency and compensation for extra call
- Signing bonuses, relocation support, and repayment terms
- Tail coverage responsibilities
- Notice periods for termination without cause
- Start dates and ramp-up expectations
Situations where you should strongly consider professional help:
- You don’t understand the compensation model or productivity formula
- Non-compete or non-solicit terms could block you from working nearby
- You’re unsure about malpractice coverage, tail, or indemnity language
- The agreement references regulatory or Stark/Anti-Kickback concerns
- You’re juggling multiple offers and want an apples-to-apples comparison
With AirCounsel’s dedicated Physician / Healthcare Contract Review, you can upload your agreement, get a line-by-line analysis from a healthcare-savvy attorney, and receive concrete negotiation suggestions—without hourly billing surprises.
Common Mistakes Physicians Make With Contracts
Even experienced physicians fall into predictable traps. Watch out for:
- Relying on verbal promises that never make it into the written contract
- Ignoring repayment language for signing bonuses, relocation, or training stipends
- Assuming tail coverage is included when you’re actually required to pay for it
- Overlooking call requirements, backup responsibilities, and holiday coverage
- Accepting “standard” non-competes without testing whether they can be narrowed
- Not planning your exit: no strategy for what happens if leadership changes or the practice is sold
Use this quick checklist of high-risk clauses:
| Clause Category | Key Questions | Risk If Mishandled |
|---|---|---|
| Duties & Locations | Are duties, sites, and hours clearly limited? | Reassignment to distant clinics or heavier call than expected |
| Compensation | Do you fully understand all formulas and metrics? | Undercompensation or surprise pay cuts |
| Non-Compete | Are radius, duration, and scope reasonable in your state? | Inability to work near your home or kids’ schools |
| Malpractice/Tail | Who pays for tail and under what conditions? | 5-figure out-of-pocket cost when you leave |
| Termination | Can either side end the contract, with realistic notice? | Sudden loss of income or malpractice coverage |
| Compliance | Does pay align with fair market value and compliance guidance? | Regulatory scrutiny, billing issues, or reputational damage |
If you spot multiple “unknowns” in these areas, that’s your signal to slow down and get a professional review before signing.
Costs, Timelines, And How Professional Review Works
Most physicians overestimate the cost and time involved in a professional physician contract review—and underestimate the cost of getting it wrong.
With AirCounsel, a typical process looks like:
- Upload your contract securely: Offer letters, full agreements, and any addenda.
- Select your tier and timing: Our Physician / Healthcare Contract Review starts at a transparent flat fee (no hourly billing), with standard 2-business-day turnaround and an optional same-day express upgrade.
- Attorney review and comments: An experienced US-licensed attorney reviews your contract, flags red/amber/green clauses, and explains risks in plain English.
- Actionable recommendations: You receive specific, suggested edits and negotiation points you can raise with your recruiter or employer.
- Optional negotiation support: If you want more help, AirCounsel’s flexible Negotiation Support option lets an attorney assist with strategy, emails, redlines, or even direct discussions with the employer.
Compared to the potential cost of an unfavorable non-compete, uncompensated call, or surprise tail bill, a flat-fee review is usually a small investment for substantial protection.
Protect Your Career With Confident Contract Review

Your physician contract shouldn’t feel like a gamble. With a structured review and clear legal guidance, you can sign knowing your income, work-life balance, and future options are protected.
AirCounsel’s flat-fee Physician / Healthcare Contract Review delivers fast, practical insights from US-licensed attorneys who understand physician employment norms, regulatory risk, and what’s realistically negotiable. If you want extra firepower at the bargaining table, our on-demand Negotiation Support and ongoing All-Access Legal Membership (USA) give you continuous, affordable access to legal advice as your career evolves.
Frequently Asked Questions
What key red flags should I watch for in physician employment contracts?
Red flags include vague duties or locations, heavily one-sided termination rights, broad non-competes (longer than 1–2 years or very wide geographic areas), unfunded tail coverage, unclear productivity formulas, and any repayment obligations that kick in if you leave early. If multiple items feel fuzzy or “trust us,” ask for clarification or legal review before you sign.
How can I ensure my compensation structure is fair and legally compliant?
Compare the offer to recent benchmarks for your specialty and region, and make sure all components—base, RVUs, bonuses—are clearly defined in writing. Watch for incentives tied directly to the volume or value of referrals, as these can raise Stark or Anti-Kickback concerns. A healthcare attorney can sanity-check both fairness and regulatory compliance.
Are non-compete clauses enforceable for physicians in the U.S.?
It depends on your state and the specific language. Some states limit or disfavor physician non-competes, while others enforce them if they are reasonable in scope, geography, and duration. Even where enforceable, non-competes can often be narrowed during negotiation. Get state-specific advice before assuming a broad non-compete is “standard” or non-negotiable.
Do I need a lawyer to review my physician contract, or can I do it myself?
You can read your contract yourself and use checklists as a starting point, but most physicians are not trained to spot subtle legal and regulatory issues. Given the stakes—compensation, license, and future mobility—many physicians choose at least a one-time professional review for their first few contracts or major career moves.
When is the best time to get my contract reviewed?
Ideally, as soon as you receive the draft agreement and before signaling you’re ready to sign. That leaves room for meaningful negotiation and revisions. You can still seek review of a signed contract (for example, when considering an exit), but you’ll have more leverage before signing.
Recommended
- Physician / Healthcare Contract Review – Flat-fee, attorney-led review tailored to physician and healthcare agreements.
- Negotiation Support – On-demand legal help to strategize and negotiate better contract terms.
- All-Access Legal Membership (USA) – Ongoing, affordable legal support for your career and practice decisions.
Need Legal Assistance?
Our expert legal team is ready to help you with contract reviews, legal advice, and more.